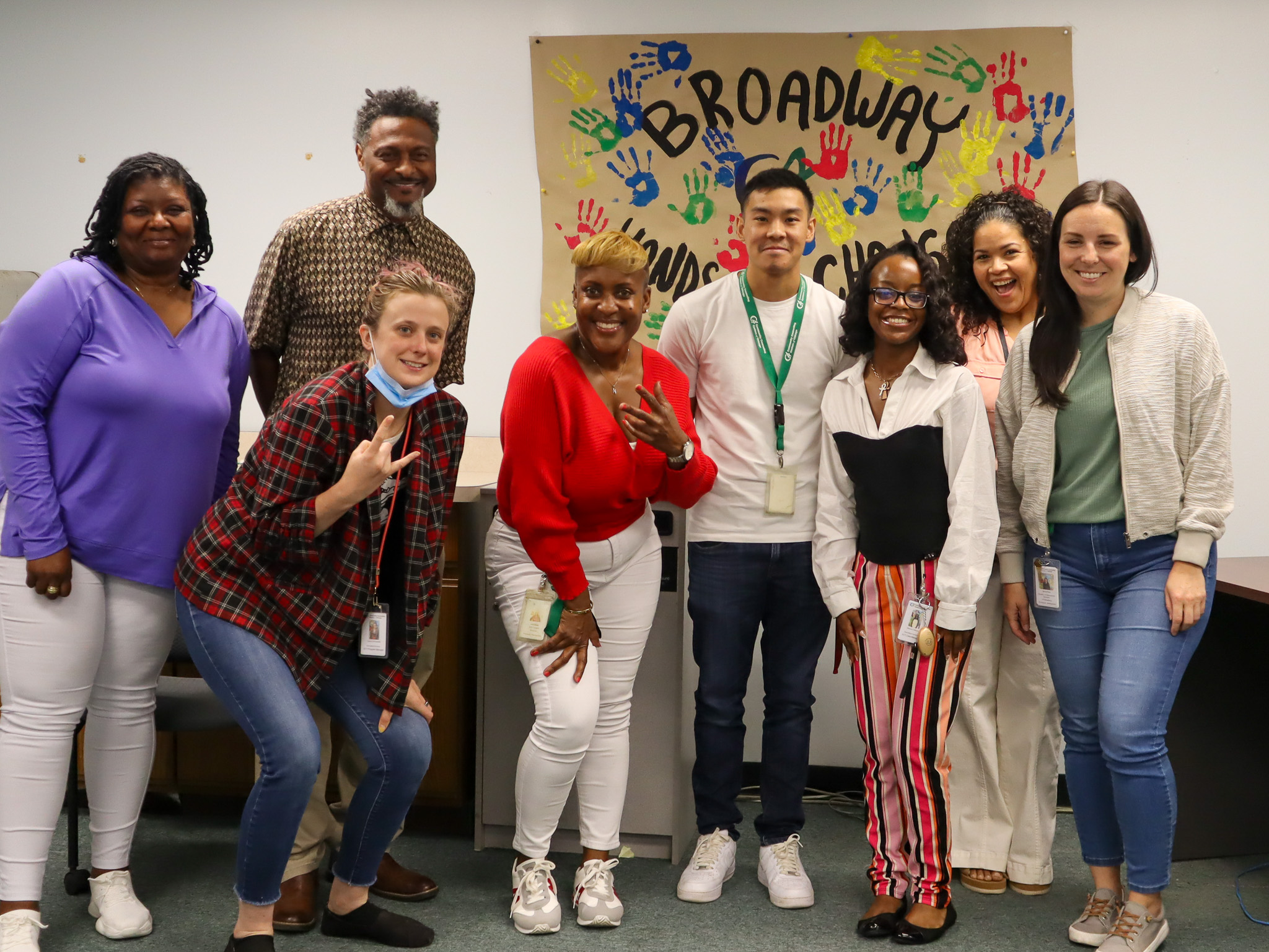News
BH-PC Collaborative talks SUD treatment strategies
The Behavioral Health Primary Care (BH-PC) Integration Learning Collaborative met Tuesday to discuss difficulties and innovations in substance use disorder treatment. The BH-PC Collaborative is a group of 35 organizations that have been working together to study and share learning on system-level issues and barriers that prevent true integration of behavioral health and primary care. C4 developed and launched the program as the lead agency in 2017.
During the meeting, Dr. Nicole Gastala, Medical Director with SUPR, shared her perspective on the state of outpatient SUD treatment, along with connecting members to systems resources. Making advancements in SUD treatment is vital – the COVID-19 pandemic exacerbated many of the mental health concerns Chicagoans already face, and substance use is no exception. In 2020, 1,302 people died of an opioid overdose in Chicago, a 52% increase over 2019 and the highest number ever recorded in the city. According to a statement from the mayor’s office, more Chicagoans now die per year from opioid overdoses than from gun-related homicides and accidents combined, highlighting the importance of systems built on engaging individuals with the comprehensive care essential to their recovery.
At the state level, substance use treatment is pivoting towards creating and sustaining recovery-oriented systems of care. This includes fostering a culture that nurtures recovery, building capacity and infrastructure, and committing to the implementation of these systems and programs.
Some recovery-oriented care systems are already underway. One evidence-backed intervention, medication-assisted recovery (MAR), involves the use of FDA-approved medications such as methadone and buprenorphine for the treatment of opiate use disorder. Compared to behavioral therapy alone, MAR decreases illicit opioid use, retains patients in treatment, and reduces mortality; patients on buprenorphine have a 40-80 percent lowered risk of fatal overdose compared to those not receiving buprenorphine treatment.
MAR NOW, which launched as a pilot program in Chicago in March and went statewide in September, is operated by BH-PC Collaborative member organization Family Guidance Centers and accessible through the existing 24/7 IL Helpline for Opioids and Other Substances. The program provides low-barrier, rapid access to buprenorphine, methadone, and naltrexone to all callers regardless of insurance status, income, ability to pay, or documentation status.
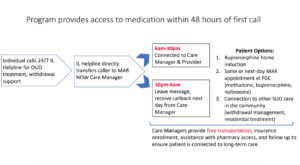
In addition to MAR NOW, IDHS is making it easier for healthcare providers to get access to naloxone (Narcan), which can now be ordered on the IDHS website and shipped to a clinic within two days.
BH-PC Collaborative providers also shared some of the setbacks they’ve been having with respect to treating SUDs. Patient engagement, staff shortages and lack of other resources were mentioned, as well as difficulties with the legal system and the expectation that clients be completely sober during treatment. Requiring sobriety to take part in treatment goes against best practices in harm reduction, but because many of the substances on which people become dependent are illegal to use, putting realistic and compassionate SUD treatment plans into practice can be challenging.
C4 only recently received a license to provide SUD services, and SUD programs are in development. We’re starting with a client and service Bill of Rights that will guide the creation of C4’s SUD programs, pursuant to a trauma-informed approach that honors the dignity and worth of each client and orients toward harm reduction. With the knowledge and experience of our peers in mind, C4 can more effectively roll out our own SUD services.